Digital health interventions are clearly something everyone at Physiopedia is passionate about, so when the WHO released their guidelines on the topic is got our interest. It’s been a few days now since the guideline has been released and that has given us time to think about how they may impact you and our profession.
The objective of the new guidelines is to highlight how technologies can help address health system challenges around the world. Yes the primary target audience for the guideline is decision makers and public health practitioners but this doesn’t mean it isn’t relevant for you or I. At a local and institutional level we can each influence what our organisations invest in.
“Harnessing the power of digital technologies is essential for achieving universal health coverage. Ultimately, digital technologies are not ends in themselves; they are vital tools to promote health, keep the world safe, and serve the vulnerable.” – WHO Director-General Dr Tedros Adhanom Ghebreyesus.
How Was The Guideline Developed?
For the exact details of how the guideline was created The WHO points readers in the direction of “the second edition of the WHO handbook for guideline development“, which is available as a PDF if you’re interested. Within the guideline itself there is a step-by-step walk through of the process which is more than detailed enough for most readers.
In essence it was developed following international online surveys, in-person consultations, a scoping meeting to prioritise and draft critical questions and outcomes, and then a final meeting to review evidence gathered and create the recommendations. Overall this took some 4 years and involved a large steering group. For evidence of the effectiveness of the interventions existing Cochrane reviews were used and if they didn’t exist new ones were commissioned. When ongoing Cochrane reviews were identified, the authors were invited to collaborate with the technical team to ensure that the reviews would be as relevant as possible for the guideline.
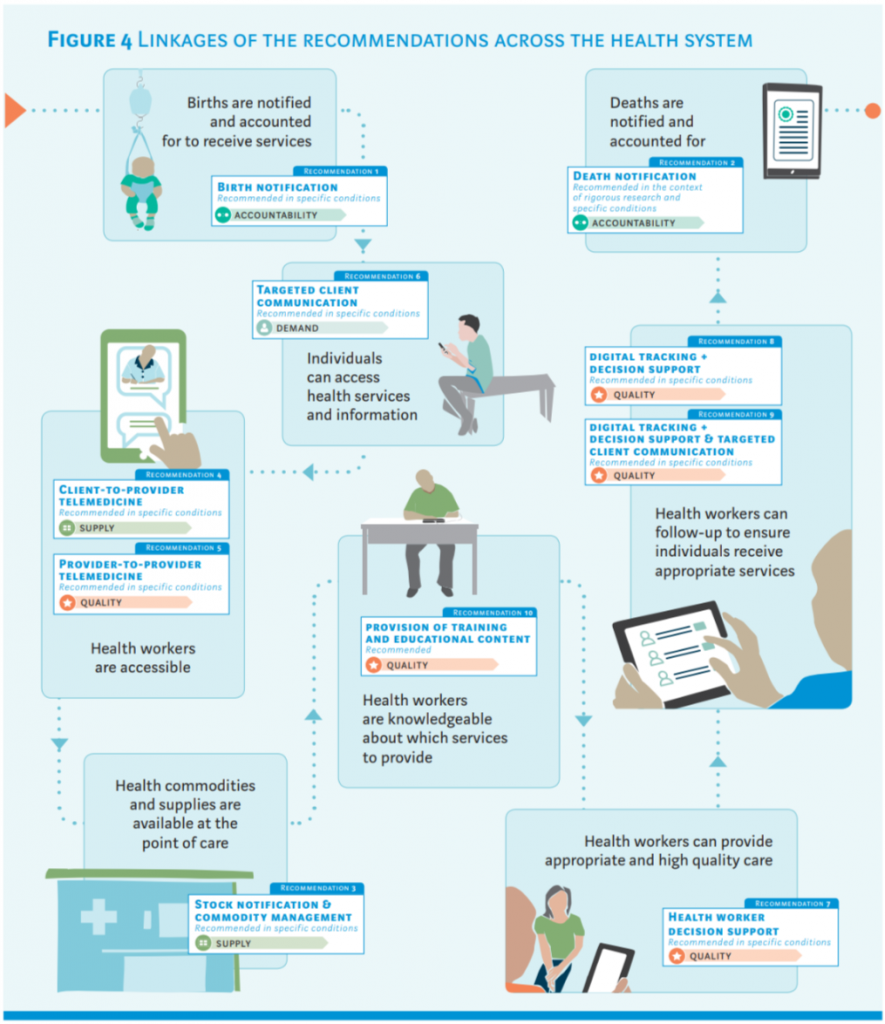
Of the 10 recommendations not all are relevant to Physiotherapy practice so let’s break it down to the ones which are.
Recommendation 4 – Client-to-Provider Telemedicine
The emphasis of this recommendation to that telemedicine should complement and not replace the delivery of health services with a view to reduce unnecessary clinical visits and improve quality of life. This is a topical subject with there being a universal shortage of healthcare workers. There are some excellent examples of where this is already happening – TEC Scotland as an example – the primary driver of the uptake of tech in this way has been about overcoming geographical boundaries particularly for rural settings. Thinking from a physio perspective it may be useful for helping patients adhere to home exercise regimes or monitoring long-term conditions such as COPD.
Recommendation 5 – Provider-to-Provider Telemedicine
As WHO explains access to qualified health workers with the appropriate competencies, skills and behaviours is an even greater obstacle to improving health outcomes than the availability of health workers. Digital approaches, most notably telemedicine between different types of health workers, have emerged as a potential way to overcome the barriers of long distances to qualified health workers and shortages in their numbers.
It may be easier to understand this recommendation with an example. Let’s say you are an MSK physio and your next patient has had a shoulder replacement. You’ve never seen this before and you are worried the patient has had a dislocation and you are unsure what to do. This recommendation is suggesting that through tech, you’ll be able to have access to a relevant specialist who will be able to give you advice. In a nutshell provider-to-provider facilitates the provision of health services at a distance and is primarily used to link less skilled health workers with more specialist ones.
It not only improves your performance but it reduces the time for your patients to receive the appropriate care and advice. Obviously safety protocols and legislation needs to be in place but once it is this will be a real advantage to most clinicians when lone-working.
Recommendation 7 – Health Worker Decision Support Accessible Via Mobile Devices
This recommendation is all about decision support tools which in a digital form are designed to aid directly in decision-making, in which characteristics of individual patients are used to generate patient-specific assessments or recommendations that are then presented to clinicians for
consideration. Functionally, decision support tools may be designed to guide health workers through algorithms and rules based on clinical protocols, provide the health worker with checklists for case management and referrals, screen clients by risk or other health status and to assist in health worker activity planning and scheduling.
An example of how this might affect your practice is the CKS by NICE – a flow chart algorithm which does what it says on the tin. Look at the Achillies Tendinopathy CKS for an example and imagine what would be possible for your own specialist areas. Then think about how worthwhile that would be for those working in low-to-middle economic areas where they are unable to access the level of training you may have had, and how transformational it would be for them to have access to decision support.
Recommendation 10 – Digital Provision of Training and Educational Content For Health Workers Via Mobile Devices/mLearning
Clearly knowledge is the target of this recommendation and the parallels between this and Physiopedia are clear and we are an active example of how eLearning is an asset to a profession. As Physiopedia and Physioplus evolve and grow the other recommendations will intertwine with our common goals and vision.
What next? – Implementation
The recommendations from this guideline need to be considered as a whole and as part of a wider solution to help combat health system needs. What you can do is talk to your managers and discuss the potential solutions, definitely point them in the direction of this guideline and spread the word as IT infrastructure is the future and can help us help our patients to get better.