1 in 2 women and 1 in 5 men over the age of 50 will break a bone as a result of osteoporosis.
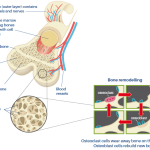
Osteoporosis means ‘porous bones’ and is a condition in which bones lose their strength. Bone is a tissue which is constantly being remodeled by our osteoblasts, which build the bone, and osteoclasts which break the bone down. When we are younger the osteoblasts work faster than osteoclasts which allows growth and increasing strength as we mature. After the age of 35 this balance tips the other way, the bone becomes increasingly thinned and the cortical shell less dense. The process is influenced by many different factors and certainly isn’t the same for everyone however, the reduction in bone density is worse for women than men.
The most severe consequence of osteoporosis is a much higher risk of fractures (often termed fragility fractures) and depending on where the fractures are, there are any number of associated consequences. For example, an older person who fractures their hip is at a much higher risk of becoming frail and immobile than someone who fractures their foot. The disease process is still the same for these two examples.
There are many ways to reduce your risk of osteoporosis and the quicker the assessment/diagnosis the more time you have to receive treatment/interventions to slow the process. These treatments are primarily pharmaceutical but also exercise is effective and should be offered as basic treatment.
When it comes to creating the best assessment and treatment plan for those with osteoporosis it can be confusing as there are a lot of options available. Not just to physiotherapists but to the wider multi-disciplinary team as well. The new NICE guidance, which is freely available, makes the process clear and can allow you to keep up to date with the latest research and understanding ensuring your patients receive the best possible care.