Running seems simple. All kids do it, so we should all do it well, right? Unfortunately, many of us develop compensations that can correlate with issues. One of these common compensations, we like to call, “The Collapser”.
The Collapser is exactly what it sounds like. Someone who conforms to the ground way too much. They absorb force in an alternative plane to the sagittal, leading to abnormal forces. How important is this?
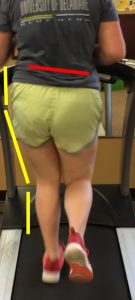 Let’s look at what a Collapser looks like first. You’ll notice the 2 hallmark signs of a Collapser (Picture to the Right): Pelvic drop and an adducted/internally rotated hip. Typically, a runner will have one or the other, but you’ll note that this runner has both. This can correlate with anterior knee pain3, lateral hip pain1, and a host of other issues.
Let’s look at what a Collapser looks like first. You’ll notice the 2 hallmark signs of a Collapser (Picture to the Right): Pelvic drop and an adducted/internally rotated hip. Typically, a runner will have one or the other, but you’ll note that this runner has both. This can correlate with anterior knee pain3, lateral hip pain1, and a host of other issues.
So back to why it is so important. When we walk, 3x our body weight goes through our knee. When we run, this is even higher. When the alignment of the knee changes such as in this runner, those loads can skyrocket. Huberti found that a 10 degree increase in dynamic Q-Angle led to a 45% increase in patellofemoral contact pressures!2 That is astronomical when you consider a typical runner can easily exceed 1500 steps per mile!
Note the yellow lines by the knee and the substantial angle the knee is currently collapsed into. That’s quite an increase in loading at the patellofemoral joint! The patient’s complaints of left anterior knee pain certainly fit together with her running form!
Now, this patient also was experiencing pain at the greater trochanter. Many would call this bursitis, which might lead to a cortisone injection, but that would not fix the mechanical flaw seen here. (The discussion of whether that injection is warranted is for another day!) Note the red line, showing the level of pelvic drop (Trendelenberg) when the patient is in left mid stance. I have seen much worse than this, but this is still problematic. The issue is that when the pelvis drops, the curve of the gluteus medius and minimus tendons around the greater trochanter change. This could lead to bursitis or tendinopathy as the undersurface of the tendons are now compressed against the trochanter and bursa.
So how can we fix this? First, we need to address any mobility problems and ensure no glute strength issues exist. Once those are completed, we need to retrain our runner. We’ll cover that in the next post!
References
- Grimaldi A, Fearon A. Gluteal Tendinopathy: Integrating Pathomechanics and Cliinical Features in Its Management. J Orthop Sports Phys Ther. 2015;45(11):910-922.
- Huberti HH, Hayes WC. Patellofemoral contact pressures. The influence of Q-angle and tendofemoral contact. J Bone Joint Surg Am. 1984;66:715-724.
- Powers C. The influence of abnormal hip mechanics on knee injury: A biomechanical perspective. J Orthop Sports Phys Ther 2010;40(2):42-51.