She worked for a national department store. It was late in the afternoon and a sales representative on the floor needed a something out of the storage room. As she entered the storage room, she quickly learned the light was burned out. Her snap decision was to walk across the dark room to the shelf to grab the needed item. The next thing she knew, she fell down through a hole in the floor. She fell through a man made hole in the floor that never had any safety installed around the outside of it. She fell 2 stories. When she gained consciousness, she was in the dark basement of the department store. She was immediately aware of severe pain. She was unable to move. She knew she either had to find her phone or die. No one would be looking for her in the basement.
Fast forward to 4 months later. Four months after her work related incident, she initiated services with me. She was referred to me after having surgery for a shoulder rotator cuff repair. When she fell, she had back pain and had shoulder/arm pain. Her story included finding her phone, calling for help and then waiting. Minutes before the emergency personnel arrived, maintenance staff found her. The maintenance men immediately dragged her away from her location as she screamed in pain and begged to be left alone. She experienced incontinence and pain in many locations of her body.
After her fall, she was transported to the emergency department. Per the emergency room physician, she did not sustain a head injury. She was just badly bruised. She was referred to a physical therapist for her shoulder pain. Her shoulder pain never improved and she was allowed to see a orthopaedic surgeon who diagnosed her with a rotator cuff tear.
This morning, Scott Buxton posted Cauda Equina Syndrome – an Update by the Experts. We learn about this in our training. We’re educated about it. We’re told that this syndrome is rare. After I read Scott’s post, I revisited Physiopedia’s page on Cauda Equina Syndrome. I found it interesting that litigation is on the rise for this supposed rare condition. The newly added video toward the end of the page is a fantastic listen.
“Betty” wanted to see me after her shoulder surgery because she knew me, trusted me and the worker compensation laws allowed her (at that point in time) to choose whoever she wanted to see. By the time she sought my services, she had easily seen a dozen or more professionals between her emergency room visit, previous physical therapy services and her own oncologist, urologist and primary care physician.
Although she had seen all these professionals, I patiently listened to her story. I wanted to know how she was doing and what had changed since her fall. Her first incontinent episode was when she fell. She now purchased pads and was unable to walk without peeing her pants. She was having difficulty with her left lower extremity: it was feeling weaker and she could no longer climb stairs normally. Her onset of back pain began immediately after the fall and was substantially better. Upon questioning, she had no idea when she was peeing her pants – just that it happened.
She had tried multiple times to tell the various medical professionals about her situation, but each was focused on the diagnosis in which she was referred.
I didn’t evaluate her shoulder that first day. I contacted her primary care physician and asked where the physician would like her to go for an MRI. I pointed out all of her symptoms, her mechanism of injury and that cauda equina syndrome needed to be ruled out. She was advised to go to the hospital emergency room or to go to a local urgent care that had an MRI machine. The patient opted for the urgent care. Upon her arrival, her MRI was scheduled 1 week later (even after reviewing my office note and recommendations). She had the MRI 1 week later. The problem list did not even include the “incidental note” of a mid sacral canal benign type II Tarlov cyst 1.6 x 2 cm.
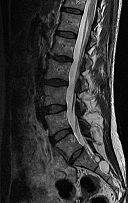 In the United States there has been a big push to downplay MRI findings. The radiologist truly believed the Tarlov cyst was “incidental,” even though the reason for the MRI was due to the fall and to rule out spinal cord compression causing incontinence. I contacted the radiologist who refused to believe the cyst was anything more than “incidental” – even with the symptoms and presentation.
In the United States there has been a big push to downplay MRI findings. The radiologist truly believed the Tarlov cyst was “incidental,” even though the reason for the MRI was due to the fall and to rule out spinal cord compression causing incontinence. I contacted the radiologist who refused to believe the cyst was anything more than “incidental” – even with the symptoms and presentation.
Because of the one word “incidental” the urologist, the oncologist and even the family care physician refused to address her situation. I was running out of all the various specialists in this lady’s life. I had to dig deep and reach out to someone I knew that had never met her. I contacted an orthopaedic surgeon who specializes in the spine. He saw her 2 days later… ordered a sacral MRI. The sacral MRI indicated 2 Tarlov cysts. He immediately referred her to a university clinic about an hour away. The second surgeon there wanted a “wait and see” approach because he didn’t have good outcomes with the surgical procedure. He did mention a surgeon in another state that is about a 6 hour plane ride.
Maybe physicians do not have time to piece together information. I had no idea what a Tarlov cyst was… but I quickly learned it could be the the result of trauma. Based on her symptoms, I knew she needed them removed to prevent irreversible damage. I truly wish I had the little information card (that is mentioned in Physiopedia) at the time I was treating this patient. Maybe the information, if presented to the specialists, would have resulted in a different response.
I full heartedly agree with the recommendations in the video on the Physiopedia page to firstly listen to your patients. Your patient has lived in his/her body far longer than anyone else. Secondly: our role is to be able to identify cauda equina syndrome suspected and cauda equina syndrome incomplete. By the time the person moves into the other two categories, it’s pretty obvious there is a significant problem. With every patient who has low back pain, I educate them on cauda equina syndrome. So many patients worry and are fearful because they don’t know when the pain will go away. They dream up worst case scenarios that are not even true scenarios. Instead, I educate them on when to worry and when to go to the emergency room. The little information card will be very helpful. I have never been that thorough with my questioning for cauda equina syndrome. My last advice: even when patients are referred to you (versus self-referral), please do not assume that previous professionals have listened or are piecing together the information provided.
To the Musculoskeletal Association of Charted Physiotherapists, I extend a big thank you! Thank you for your efforts to help us improve our care and improve our communication with our patients.