Team Work
My first encounter of working as member of a team with other health professionals was after graduating from University of Ghana. This team comprised doctors, pharmacists and nurses. Being my first Multidisciplinary Team (MDT), I struggled finding my place within the team, knowing how and when to contribute, and understanding the dynamics of achieving MDT goals. I couldn’t keep up with the team, because I felt I could contribute more within the physiotherapy unit, than with the team.
Team work is very vital to achieving the Rehab 2030 agenda. MDT work was part of the ten key areas of commitment during the call for action. Participants were committed to ‘Developing a strong multidisciplinary rehabilitation workforce that is suitable for country context, and promoting rehabilitation concepts across all health workforce education’.
MDT, although is core to the practice of health professionals and rehabilitation, hasn’t been adequately engraved into the learning pathway of most health professions in developing countries.
As a physiotherapist, I was trained with my colleagues and learned how to work effectively with other physiotherapists and within my unit, but not necessarily how to work with other health professionals.
According to Tuckman’s stages of team development (Forming, Storming, Norming & Performing), I found myself in the forming stage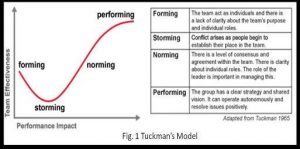 , as did most of my colleague who had the opportunity to work with other professionals. Most successful physiotherapy and rehabilitation programs in Ghana have strong MDT approach, especially in rural areas where access to rehabilitation can be very difficult.
, as did most of my colleague who had the opportunity to work with other professionals. Most successful physiotherapy and rehabilitation programs in Ghana have strong MDT approach, especially in rural areas where access to rehabilitation can be very difficult.
How can we ensure that rehabilitation professionals (PT, OT, SLP etc.) in developing countries can overcome the challenges of MDT? A different approach to the training of health professionals could help address some of these challenges.
An example of interprofessional and interdisciplinary teaching and learning is the ‘Interprofessional Learning Pathway Framework’ at the University of Alberta (link). This framework brings together the training of all health students from different faculties within the University on four core interprofessional competencies;
- Communication: Communication skills that enhance interprofessional team function
- Collaboration: Interprofessional team process skills that achieve common goals
- Role Clarification: Understanding of own role and the roles of others in an interprofessional context
- Reflection: Critical evaluation of professional and team practice in an interprofessional context
Although this model might not work for all developing countries, it is one of the ways of ensuring effective MDT from classrooms to practice. Experimenting and adopting such models could help in developing strong MDT workforce and help in achieving the Rehabilitation 2030 agenda.
WHO projects and other health projects in developing countries could place some emphasis on Interprofessional training and learning. Strong and effective rehabilitation teams could mitigate some challenges to rehabilitation in developing countries including the lack of awareness of such professionals, delayed referrals to the appropriate professionals and rapid management of complications.
MDT is vital to achieving the Rehabilitation 2030 agenda, which is key to attaining Universal Health Coverage for developing countries. The final part of this series will focus on how ‘Appropriate Technology’ can help in strengthening rehabilitation for developing countries.