There are few things that bring more debate than the SI Joint (SIJ) when discussing musculoskeletal disorders. It seems there are 2 opposing sides:
- The SI Joint only moves 4 degrees so it almost never is a contributor to a patient’s pain.
- SI Joint asymmetry is found in many patients with pain and many of these patients can be diagnosed with some sort of SI Joint problem.
While these camps continue to debate the subject, like most things in life, the answer probably lies somewhere in the middle. If it was never a problem then the second camp likely would have been phased out. If it was always the problem, then the first camp would have seen the light by now. So how can we start to understand this problem better?
Let’s start with a thought, not all SI Joint problems are created equal. There’s a thought that has been presented, which creates much more clarity to the issue. When we discuss the SIJ, we really need to adjust our terminology and separate it into 2 separate (but sometimes related) issues.
- SI Joint Pain
- SI Joint Dysfunction
SI Joint Pain
SI Joint pain occurs when the SI joint is the driver of someone’s nociceptive input. In those cases, you should be able to reproduce the pain with a provocation test and reduce the pain with a lidocaine injection or a test aimed at reducing symptoms. We treat the rest of the body in this manner. If someone has shoulder impingement, we attempt to recreate the impingement and illicit pain. If someone has a painful hip joint, then provocative testing of the hip should recreate the pain. Why would the SI Joint be so different? If the SI Joint is painful, then we should be able to provoke the pain with our testing.
Mark Laslett did a fantastic job of this with his study showing that 3 positive provocation tests led to an improved likelihood ratio of finding pain relief with a lidocaine injection.4 There was a second, similar study publish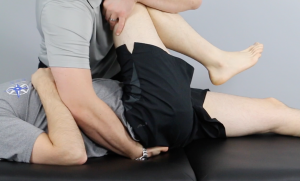 ed by van der Wurff, indicating similar results with similar likelihood ratios.7
ed by van der Wurff, indicating similar results with similar likelihood ratios.7
(+) SI Provocation testing provides a likely diagnosis of SI Joint Pain
SI Joint Dysfunction
SI Joint Dysfunction is a bit more confusing in my eyes. Dysfunction occurs when there is altered SI Joint movement through side-to-side asymmetry. This often leads to the diagnosis of the SI Joint in the presence of pain in the back. This certainly can be a contributing factor, but if we can’t provoke the SI Joint and create the pain, then it likely isn’t the source of pain. This does not mean it’s not important though! It certainly can be in many instances.
Many individuals experience anterior knee pain due to altered mechanics at the hip or ankle.5 Others experience shoulder pain due to poor scapular mechanics.6 In each of these cases, we likely need to address the joints around the region of pain, but it doesn’t necessarily mean that this is the only pain or the actual tissue resulting in nociception.
So let’s consider whether there’s actually any evidence to support this idea…..
Mike Cibulka did a great job of presenting this literature in the early 90’s. He first published a brief, but fantastic look into hip pain in runners and documented that treating SI Joint Asymmetry with a manipulation led to better outcomes than mobilizing the hip joint!1 (I have written about this incredibly important finding previously when discussing how to treat hip pain in athletes) Cibulka also documented positive findings with the same manipulation in many individuals with back pain.2 This same manipulation was later used by Tim Flynn during the development of the well-known manipulation Clinical Prediction Rule.3
Summary
There are 2 sides who are often at odds in the SI Joint discussion, but as we look at the literature and our own patient results, I am confident we can all find common ground. The first step is to begin treating the SI Joint like every other region of the body. We can treat a non-painful region to help something else (SI Joint Dysfunction). We can also treat a painful region to help itself in the presence of pain provoked with testing (SI Joint Pain).
Whether you are in one camp or the other, it is important to challenge yourself and keep an open mind. We all owe it to our patients! If you haven’t considered these details before, there’s no better time than now!
Looking for more ideas on running, rehab, and thought provoking ideas? Follow me on Twitter.
- Cibulka MT, Delitto A. A comparison of two different methods to treat hip pain in runners. J Orthop Sports Phys Ther. 1993;17(4):172-176.
- Cibulka MT, Koldehoff R. Clinical usefulness of a cluster of sacroiliac joint tests in patients with and without low back pain. J Orthop Sports Phys Ther. 1999;29(2):83-92.
- Flynn T, Fritz J, Whitman J, et al. A clinical prediction rule for classifying patients with low back pain who demonstrate short-term improvement with spinal manipulation. Spine. 2002;27:2835.
- Laslett M, Aprill CN, Mcdonald B, Young SB. Diagnosis of Sacroiliac Joint Pain: Validity of individual provocation tests and composites of tests. Manual Ther. 2005;10:208-218.
- Powers C.The influence of abnormal hip mechanics on knee injury: A biomechanical perspective. J Orthop Sports Phys Ther 2010;40(2):42-51.
- Solem-Bertoft E, Thuomas KA, Westerberg CE. The influence of scapular retraction and protraction on the width of the subacromial space. An MRI study. Clin Orthop Relat Res. 1993;296:99-103.
- van der Wurff P, Buijs EJ, Gerbrand JG. A Multitest Regimen of Pain Provocation Tests as an Aid to Reduce Unnecessary Minimally Invasive Sacroiliac Joint Procedures. Arch Phys Med Rehabil. 2006;87(1):10-14.