In Part 1 of Athletic Hip Pain I discussed how I found a niche for treating athletes with hip pain after understanding Cibulka’s1 literature of manipulating the SI Joint/Lumbar spine. In part 2, I want to expand on this and discuss 2 cases of patients I recently treated.
Case 1
The first case was exactly like my previous. I evaluated the patient. I manipulated the patient. They got better very quickly. Everyone was happy.
Case 2
The second case started out like the others. I evaluated the patient. I manipulated the patient. There was no change in symptoms. This is where the impact occurs beyond where the immediately applicable literature would lead us.
The first thing to recognize is the common pattern that occurs in these athletes. Janda’s cross syndrome states there is often hypertonic anterior hip musculature with inhibition of posterior hip musculature. What would make sense is that we would stretch the anterior hip and strengthen the posterior hip. Unfortunately, these patients are often difficult and many times it is not that easy.
Here’s the test I like to use. I have the patient perform side lying hip abduction, prone hip extension, or even a bridge. I then assess by looking, listening, and feeling.
- Look: I watch the patient and note any abnormal compensatory motions
- Listen: I ask the patient where they are feeling the contraction of muscles
- Feel: I palpate what is contracting. Is it what I expect or is there a compensation?
Often what we find with these patients is that not only are they weak, but there is an abnormal muscle firing pattern and core stability issues. Let’s start with core stability.
Core stability is often thought of as planks and sit-ups, or some other variation of these activities. What the core is really responsible for is providing a stable base for the hip musculature to attach. I describe it to patients in this manner:
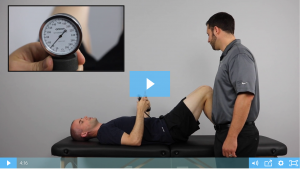
Imagine you are firing a cannon off a canoe. Will the cannon ball fire forward or will the canoe shoot backwards? This is what occurs when our hip moves on an unstable core. Instead of the hip moving with a strong base, the pelvis tilts, twists, and deforms to the load. So how do we fix it? Assuming there are no substantial mobility impairments, a great way of fixing this is to use a biofeedback device (such as a blood pressure cuff) and ensuring your patient understands why you are stressing this small movement. You can watch us discussing this during a small excerpt from the ACE Online Hip Course in the video below.
 The other issue we discussed is an abnormal firing pattern. This won’t make sense until you look, listen, and feel with your patients. Try having some of these patients perform a side lying hip abduction and assess. You would expect the gluteus medius and minimus to contract, but often you will notice these individuals fire their TFLs and hip flexors. This can be a complicated issue, but we can fix it!
The other issue we discussed is an abnormal firing pattern. This won’t make sense until you look, listen, and feel with your patients. Try having some of these patients perform a side lying hip abduction and assess. You would expect the gluteus medius and minimus to contract, but often you will notice these individuals fire their TFLs and hip flexors. This can be a complicated issue, but we can fix it!
Let’s use the TFL as an example. The TFL’s actions are typically described to be hip flexion, abduction, and internal rotation. The gluteus medius actions are hip abduction, extension, and external rotation. What if we were to force the gluteus medius to contract, resulting in TFL inhibition? We can do that! We can take advantage of reciprocal inhibition in these patients. If the patient isometrically pushes into hip extension (gluteus medius) and maintains this throughout side lying hip abduction (or a side lying clam), the TFL has no choice but to relax.
These 2 steps are 2 of the primary steps I used in case 2 to get results with my athlete with hip pain. Of course, there were mobility impairments and we also progressed well past these simple table exercises, but these laid the foundation for a successful progression.
Try these out with your athletes with hip pain this week and let me know how it goes! If you’re interested in hearing more, check out our YouTube Page for mobility drills or Hip Pain: Complete Management from Start to Finish – Part 1 (approved for PTs/PTAs in MD, DE, PA; Approved Nationwide for Athletic Trainers).
- Cibulka MT, Delitto A. A comparison of two different methods to treat hip pain in runners. J Orthop Sports Phys Ther. 1993;17(4):172-176.