A new systematic review suggests that surgery provides better outcomes for people with symptomiatic FAI when compared to physiotherapy alone. However a combined approach of physio and surgery provides best long term outcomes.
In this post we will explore this systematic review and see what conclusions can be drawn from the systematic review and what changes we need to make to our clinical practice.
What is Femoroacetabular Impingement?
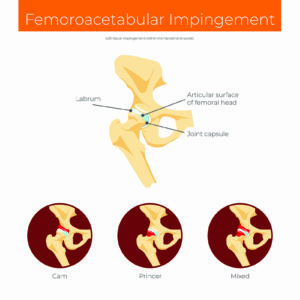
Femoroacetabular impingement syndrome (FAI) is a motion-related disorder of the hip involving premature contact between the acetabulum and the proximal femur causing pain and dysfunction. There are different types of FAI which can be divided into three different morphologies. A CAM impingement describes a flattening or convexity of the femoral head and is more common in men. A PINCER describes an overcoverage of the femoral head by the acetabulum where the acetabular rim extends beyond the typical amount either generally or focally and is more common in women. The third type is thought to be the most common (although this is debated) and is a MIXED type with elements of both cam and pincer impingement.
Target Your Hip and Knee Exercises
These morphologies are thought to be fairly common in the general population however only a fraction of them go on to become problematic and develop FAI syndrome. According to one systematic review the development of the syndrome is likely multifactorial so presence of the morphology alone doesn’t mean pain and impairment will develop.
There is debate about what the best management strategy is for FAI. The most common treatment is arthroscopic surgery which involved reshaping or trimming the bones dependent on the morphology of the impingement. However there are some limitations of the surgery in that hip ROM in frontal plane does not improve resulting in continued impairment in activities such as climibng stairs. This is one of the key roles of physiotherapy in the management of FAI with hip and knee strengenthing playing crucial parts in improving functional outcomes post surgery.
Some studies suggest that conservative management provided patients with as good if not better outcomes to surgery. In particular Casertelli et al (2016) and the UK FASHIoN Trial trial suggest individualised hip and knee strengthening and proprioception exercises provide good outcomes and prevent the need for surgery therby reducing exposure to surgical complications.
A new systematic review published in the Orthopaedic Journal of Sports Medicine this week has tried to further our understanding of which approach should be taken for FAI; a conservative or surgical approach. This review has specifically aimed to investigate short-term outcomes.
Methodology of the Systematic Review
This systematic review does a reasonable job in reporting the methodological approach used. The PRISMA guidelines were adhered to by the authors of the paper and the search strategy and research question are clearly available to the reader however more could have been done to publish the search strategy in full. A brief shortened version of the key words used is available which is disappointing as it prevents critique. The databases used for the review goes above and beyond the Cochrane recommendations which is good to see and a transparent process is available to see in the PRISMA flow chart
The research question this systematic review aimed to answer was:
“Is there a difference in patient reported outcomes of patients with femoroacetabular dysplasis impingement who have surgery versus conservative management with physical therapy?”
 Study selection and data collection is written in more detail than the search strategy allowing appropriate scope to evaluate the process. Only two reviewers were used to extract and select the studies used within the review instead of the recommended three. This means there wasn’t a third reviewer available to provide judgement if there was disagreement between the two reviewers. It’s unclear what the two did if there was a disagreement.
Study selection and data collection is written in more detail than the search strategy allowing appropriate scope to evaluate the process. Only two reviewers were used to extract and select the studies used within the review instead of the recommended three. This means there wasn’t a third reviewer available to provide judgement if there was disagreement between the two reviewers. It’s unclear what the two did if there was a disagreement.
CONSORT, TIDieR, CERT and the Cochrane Risk of Bias Tool were all used to ensure evidence based requirements for both physio and surgical trials as well as assessing for risk of bias. in total three (n=3) studies were used within the review incorporating outcomes for 650 patients. Two of the studies were assessed as good with minial risk of bias whereas one was deemed to have a high risk of bias due to poor reporting and a single centre cross over trial design. All studies we unable to be blinded due to the type of procedures being assessed.
It is worth considering that all of the studies had a long wait between being randomisation to surgery (~3 months) and short term outcomes were assessed relative to time of randomisation. None of the included studies involved the now popular capsular closure surgical procedure which initial studies show improves outcomes compared the the approaches used within this systematic review.
Outcomes and Analysis
The outcome measures used within the review were the iHOT-33 (all three studies), HOS-ADL and HOS-Sport. Enough heterogeneity of results allowed a meta-analysis to be perfomed with a SMD.
 Looking specifically at the physiotherapy interventions there is a lot of variation and no standardisation in treatment choice in the included studies. Commonalities in apporach include home exercise plans which consist mainly of hip strengthenign and neuromuscular control and education sessions which emphasise avoiding the impingement position.
Looking specifically at the physiotherapy interventions there is a lot of variation and no standardisation in treatment choice in the included studies. Commonalities in apporach include home exercise plans which consist mainly of hip strengthenign and neuromuscular control and education sessions which emphasise avoiding the impingement position.
Overall surgery improves iHOT-33 and HOS-ADL scores more than physiotherapy alone. There was no difference in outcome between the treatment groups at 6 months follow up. Those that crossed over from physiotherapy to surgery had better outcomes than either single treatment group.
Clinical Implications
There is not enough evidence high quality unbiased date to be able to draw definitive conclusions in answering this specific research question. What we can say is that as things stand, surgery with post-operative physiotherapy which focusses on hip and knee proprioception and strengthening exercises provides best patient outcomes. There is also evidence which supports the used of education sessions which aim to prevent patients from going into an impingement position.
